The effects of long acting and different doses of Danofloxacin on oxidative stress, biochemical, and hemogram parameters in rats
Abstract
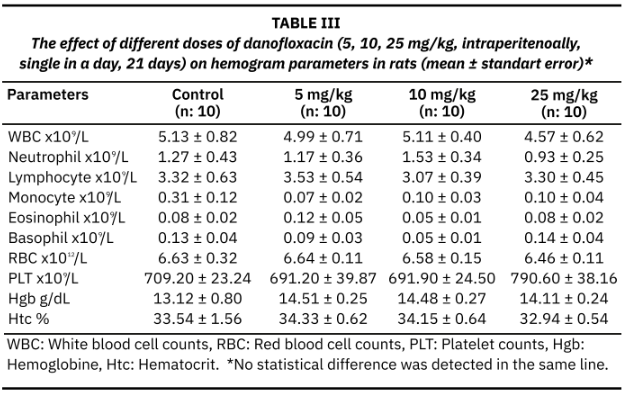
Danofloxacin is a new generation fluoroquinolone antibiotic. There is limited literature information regarding its toxicity with long-term use. Therefore, likelihood of adverse effects increases. This study was aimed to determine the effects of long-term danofloxacin administration at different doses primarily on serum oxidative stress parameters, as well as biochemical and complete blood count parameters. Forty rats were divided into four groups with equal numbers in each group. While rats in the control group were not subjected to any treatment, other three groups received 5, 10, and 25 mg/kg of danofloxacin (intraperitoneal) daily for three weeks, respectively. At the end of the experiment, the animals were anesthetized, blood samples were collected and they were euthanized. The collected blood samples were centrifuged to separate the serum fractions. Serum levels of oxidative stress parameters (malondialdehyde, superoxide dismutase, glutathione peroxidase) were determined using the Enzyme - Linked Immunosorbent Assay reader. Levels of serum biochemistry parameters (aspartate aminotransferase, gamma glutamyl transferase, blood urea nitrogen, cholesterol, phosphorus, magnesium) were measured using an autoanalyzer. Hemogram parameters (white blood cell, red blood cell, platelet, hematocrit, hemoglobin) were measured using a hemocell counter device. In the study, administration of danofloxacin for 21 days at different doses had no effect on oxidative stress and hemogram parameters (P > 0.05). However, high doses (10 and 25 mg/kg) of danofloxacin elevated aspartate aminotransferase, gamma glutamyl transferase, cholesterol, and phosphorus levels (P < 0.05). In conclusion, long-term administration of danofloxacin does not cause oxidative stress or affect hemogram parameters; however, patients should be monitored for liver and kidney function and lipid metabolism. Furthermore, more studies using histopathological or molecular methods involving disease models are needed to determine the extent of organ damage in the future.
Downloads
References
Yazar E. Veteriner İlaç ve Aşı - A dan Z ye (2018-2019). 1 Cilt. Ankara, Türkiye: Nobel Tıp Kitabevleri; 2018.
Yazar E. Kemoterapi. Yazar E, editör. Veteriner İlaç Rehberi Tedavi El Kitabı,. Ankara, Türkiye: Nobel Tıp Kitabevleri; 2024. 85-130.
Jessen LR, Sorensen O, Bjornvad CB, Nielsen SS, Guardabassi L. Effect of antibiotic treatment in canine and feline urinary tract infections: A systematic review. Vet. J. [Internet]. 2015; 203(3):270-277. doi: https://doi.org/f66tmg
Bauscha K, Bonkat G. Fluoroquinolone antibiotics - what we shouldn't forget two years after the restriction by the European Commission. Swiss Med. Wkly. [Internet]. 2022; 152(0304):w30126. doi: https://doi.org/qx2d
Cekic O, Aydin UT. Fluoroquinolone use and the risk of retinal detachment. Ret. Vit. [Internet]. 2014 [cite 22 Dec 2025); 22:324-327. Available in: https://goo.su/mqFt2J0
Coskun D, Parlak K, Dik B, Faki HE, Bahcivan E, Yazar E, Er A. Effect of enrofloxacin on the joint fluid/blood oxidative status and organ damage markers. Annu. Res. Rev. Biol. [Internet]. 2018; 25(3):1-7. doi: https://doi.org/qr9d
Pouzaud F, Bernard-Beaubois K, Thevenin M, Warnet JM, Hayem G, Rat P. In vitro discrimination of fluoroquinolones toxicity on tendon cells: involvement of oxidative stress. J. Pharmacol. Exp. Ther. [Internet]. 2004; 308(1):394-402. doi: https://doi.org/btg5q6
Yazar E, Tras B. Free oxygen radicals, antioxidant enzymes and antibiotics. J. Turk. Vet. Med. Assoc. [Internet]. 2002; 14:42-44.
Ozcan O, Erdal H, Cakirca G, Yonden Z. Oxidative stress and its impact on intracellular lipids, proteins and DNA. J. Clin. Exp. Invest. [Internet]. 2015; 6(3):331-336. doi: https://doi.org/p4zh
Ball P, Tillotson G. Tolerability of fluoroquinolone antibiotics. Past, present and future. Drug Saf. [Internet]. 1995; 13(6):343-358. doi: https://doi.org/b4nmhv
Nakamura S. Veterinary use of new quinolones in Japan. Drugs. [Internet]. 1995; 49:152-158. doi: https://doi.org/crzg4g
Montagnac R, Briat C, Schillinger F, Sartelet H, Birembaut P, Daudon M. Fluoroquinolone induced acute renal failure. General review about a case report with crystalluria due to ciprofloxacin. Nephrol. Ther. [Internet]. 2005; 1(1):44-51. doi: https://doi.org/dvkbgr
Uslu M, Yazar E. Side effects of fluoroquinolones in cats and dogs. Euro Asia 10th International Congress on Applied Sciences; 2022 Aug 7-9; Ankara, Türkiye. Ankara: Yozgat Bozok University; 2022. p. 159-163. Available in: https://goo.su/VM1vbvq
Food and Drug Administration (FDA). FDA warns about increased risk of ruptures or tears in the aorta blood vessel with fluoroquinolone antibiotics in certain patients. [Internet]. FDA Drug Safety Communication. Montgomery, Maryland, USA: FDA. 2019 [cited 22 Nov 2025]. Available in: https://goo.su/eUOwjcB
Kaya S, Ünsal A. İlaçların istenmeyen etkileri [Adverse effects of medications]. In: Kaya S, Pirinçci İ, Bilgili A, editors. Veteriner Hekimliğinde Farmakoloji. 3rd ed. Ankara, Türkiye: Medisan; 2002. p.142-152.
Dogan F. Veteriner hekimliğinde farmakovijilans. Eurasian J. Vet. Sci. [Internet]. 2011 [cited 22 Oct 2025]; 27(1):19-25. Available in: https://goo.su/jy92MPL
Turgut K. Karaciğer testleri. Veteriner Kliniği Laboratuvar Teşhisi. Konya, Türkiye: Bahçıvanlar Matbaası; 2000. p. 153-257.
Kerr MG. Clinical biochemistry. Veterinary Laboratory Medicine, Clinical Biochemestry and Haematology. 2nd ed. London, UK: Blackwell Science; 2002 [cited 22 Oct 2025]. p. 69-196. Available in: https://goo.su/re7hE8Y
Turgut K. Lipid metabolizması bozuklukları ve testleri. Veteriner Kliniği Laboratuvar Teşhisi. Konya, Türkiye: Bahçıvanlar Matbaası; 2000. . 408-416.
Turgut K. Endokrin, metabolik ve lipid bozukluklarının testleri. Veteriner Kliniği Laboratuvar Teşhisi. Konya, Türkiye: Bahçıvanlar Matbaası; 2000. р. 416-486.
Celkan TT. What does a hemogram say to us? Turk. Pediatri. Ars. [Internet]. 2020; 55(2):103-116. doi: https://doi.org/gnpq
Coskun D, Dik B, Korkmaz Y, Canbar R, Er A, Yazar E. Investigation of cardiotoxic effects of marbofloxacin. Eurasian J. Vet. Sci. [Internet]. 2019; 35(2):56-61. doi: https://doi.org/qx2z
Coskun D, Yazar E. Kedilerde ve köpeklerde pradofloksasin kullanımı. MAS 13th International European Conference in Mathematics, Engineering, Natural & Medical Sciences; 2020 Oct 23-25; Faryab, Afghanistan. Ankara: Afghanistan, Faryab University; 2020. p. 50-56. Available in: https://goo.su/NcywUU
Gorris F, Faut S, Daminet S, Rooster H, Saunders JH, Paepe D. Pyothorax in cats and dogs. Vlaams Diergeneeskund. Tijdschr. [Internet]. 2017; 86(3):183-197. doi:https://doi.org/qx22
Newton PL, Fry DR. Successful treatment of Providencia rettgeri cholecystitis and neutrophilic cholangitis in a cat. J. Feline Med. Surg. Open Rep. [Internet]. 2018; 4(1):2055116917750763. doi: https://doi.org/qx23
Yazar E, Tras B. Effects of fluoroquinolone antibiotics on hepatic superoxide dismutase and glutathione peroxidase activities in healthy and experimentally induced peritonitis mice. Revue Med. Vet. [Internet]. 2001 [cite 11 Nov 2025] ; 152(3):235-238. Available in: https://goo.su/Ril5ed
Kumbhar GB, Khan AM, Rampal S. Evaluation of gatifloxacin for its potential to induce antioxidant imbalance and retinopathy in rabbits. Hum. Exp. Toxicol. [Internet]. 2015; 34(4):372-379. doi: https://doi.org/f68brx
Elbe H, Dogan Z, Taslidere E, Cetin A, Turkoz Y. Beneficial effects of quercetin on renal injury and oxidative stress caused by ciprofloxacin in rats: A histological and biochemical study. Hum. Exp. Toxicol. [Internet]. 2016; 35(3):276-281. doi: https://doi.org/f79rtd
Kuula LSM, Backman JT, Blom ML. Healthcare costs and mortality associated with serious fluoroquinolone-related adverse reactions. Pharmacol. Res. Perspect. [Internet]. 2022; 10(2):e00931. doi: https://doi.org/qx26
Baggio D, Ananda-Rajah MR. Fluoroquinolone antibiotics and adverse events. Aust. Prescr. [Internet]. 2021; 44(5):161-164. doi: https://doi.org/jmh4
Tsai WC, Yang YM. Fluoroquinolone-associated tendinopathy. Chang Gung Med. J. [Internet]. 2011 [cited 11 Dec 2025]; 34(5):461-467. Available in: https://goo.su/598UR70
Coskun D, Canbar R, Korkmaz Y, Dik B, Er A, Yazar E. Determination of the effect of danofloxacin on 8-hydroxy-2-deoxyguanosine level. Eurasian J. Vet. Sci. [Internet]. 2019; 35(4):224-229. doi: https://doi.org/qr9f
Tras B, Maden M, Bas AL, Elmas M, Yazar E, Civelek T. Investigation of biochemical and haematological side-effects of enrofloxacin in dogs. J. Vet. Med. A. [Internet]. 2001; 48(1):59-63. doi: https://doi.org/c7qt5r
Licata A, Randazzo C, Morreale I, Butera G, D'Alessandro N, Craxi A. Fluoroquinolone-induced liver injury: three new cases and a review of the literature. Eur. J. Clin. Pharmacol. [Internet]. 2012; 68(5):525-532. doi: https://doi.org/fxrzvs
Maddix DS, Warner L. Do we need an intravenous fluoroquinolone? West J. Med. [Internet]. 1992; 157(1):55-59. PMID: 1413744. Available in: https://goo.su/OJliu50